Meet Shannon: NICU Twin mom navigating the unknown
Welcome to Coco’s Caravan Community. I started this community in hopes of helping others. After sharing my story and hearing back from so many others who were dealing with similar trials, I realized we are not alone. We are here to uplift and help each other make it through each day. I hope by sharing their stories it can help you in some way. Continue reading below to learn more about Shannon’s story below!

Table of Contents
Shannon’s Story: NICU Twin Mom
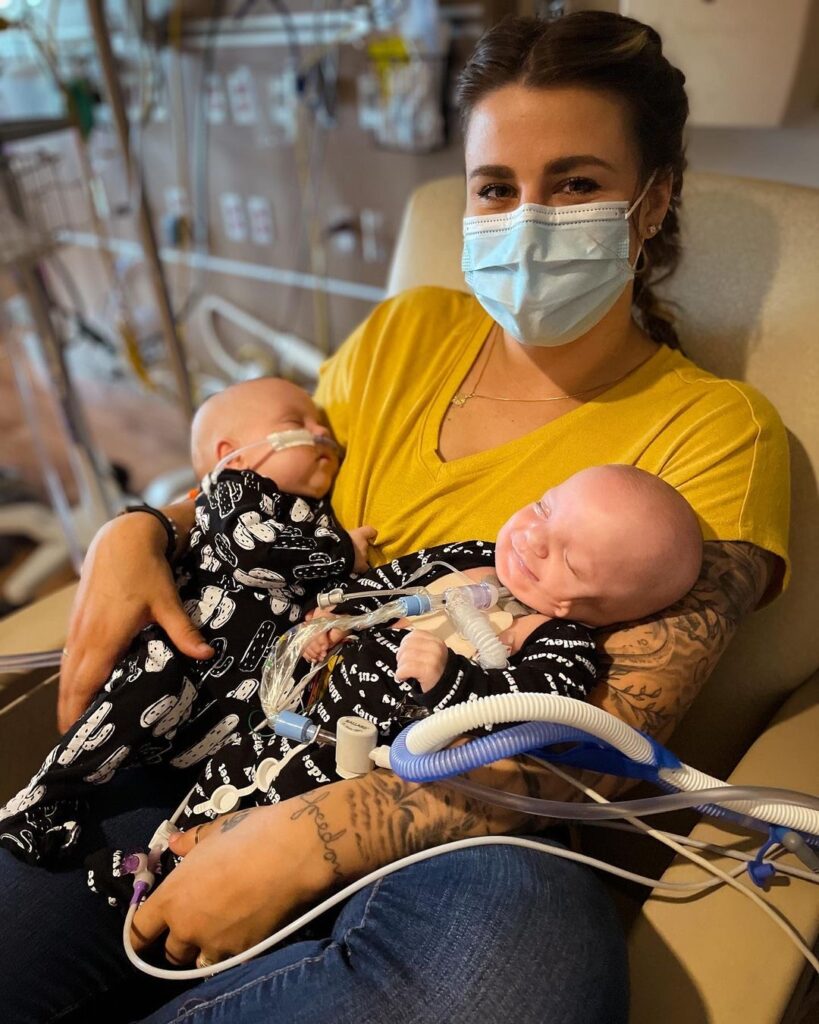
Summer of 2020 was full of adventures and love with my husband and our thriving 18 month old. We finally felt that we were at a point in our new parental journey to begin trying for our next child. We were very fortunate because as soon as we started trying we got a positive pregnancy test. I contacted my mid-wife regarding the positive test and she asked me to come in around my estimated 8 week mark.
At the appointment she suggested getting an ultrasound just to see how far along I actually was and who wouldn’t want to see their little babe on the monitor! We were deep into COVID at the time, so my husband was unable to come to the appointment. This was our second child so I felt ok to be on my own. The ultrasound tech took me back and I had all those normal anxious feelings as she found the baby and began to assess the heartbeat.
She then stopped and my heart sank, thinking of the worst possibilities. Hearing the word twins was not one of the possibilities I had in mind. I started to laugh and cry, I was in utter shock. I then started to think about what Jack my husband was going to say. We have no history of twins in our family. As she begin to wrap up our appointment she said “well it looks like mono-mono twins” and that was it. She set up our next appointment with Maternal Fetal Medicine where I would be closely monitored my entire pregnancy.
I was anxious for my follow up appointment with my mid-wife. I had gone down the rabbit-hole on the internet researching the survival rate of mono-mono twins. I was devastated at what I was finding. We got some hard news at my 16 week ultrasound that one of our boys had a heart defect and I was sent to see a cardiologist. After the appointment we left with not one diagnose but two, both boys had a heart defect. It felt like the hits just kept coming, I was once again crushed thinking how on earth is this happening to me. This is something that you read about or see on social media, this doesn’t happen to me.
On top of all of this, my husband and I received the information that I had to do an inpatient stay after we reached the point of viability (24 weeks). I would have to move into the hospital until the boys where delivered and be under constant monitoring. This news was extremely hard to take. How could I leave my 18 month old son for potentially 2 1/2 months until a safe time to deliver. I felt like I was choosing between my children, but we knew it would be safest for the twins if I went into the hospital at 25 weeks.
After 20 weeks I got pushed to one ultrasound a week and finally got some good news. One of our boys heart defect resided on its own, praise God that it was something that wouldn’t need correcting and he could live a totally normal life!
It came time to check into the hospital. It was strange because I wanted it to come up fast, but I also wanted time to slow down so I didn’t have to leave Easton (my 18 month old). I tucked Easton into bed and kissed him for what felt like the last time, I sobbed uncontrollably the whole drive to the hospital. Due to COVID I was unable to see him or leave the hospital to even go outside for a visit. I could only have one visitor which was my husband, but he was not able to come up all the time because he had to work and try to keep our household as normal as possible for Easton.
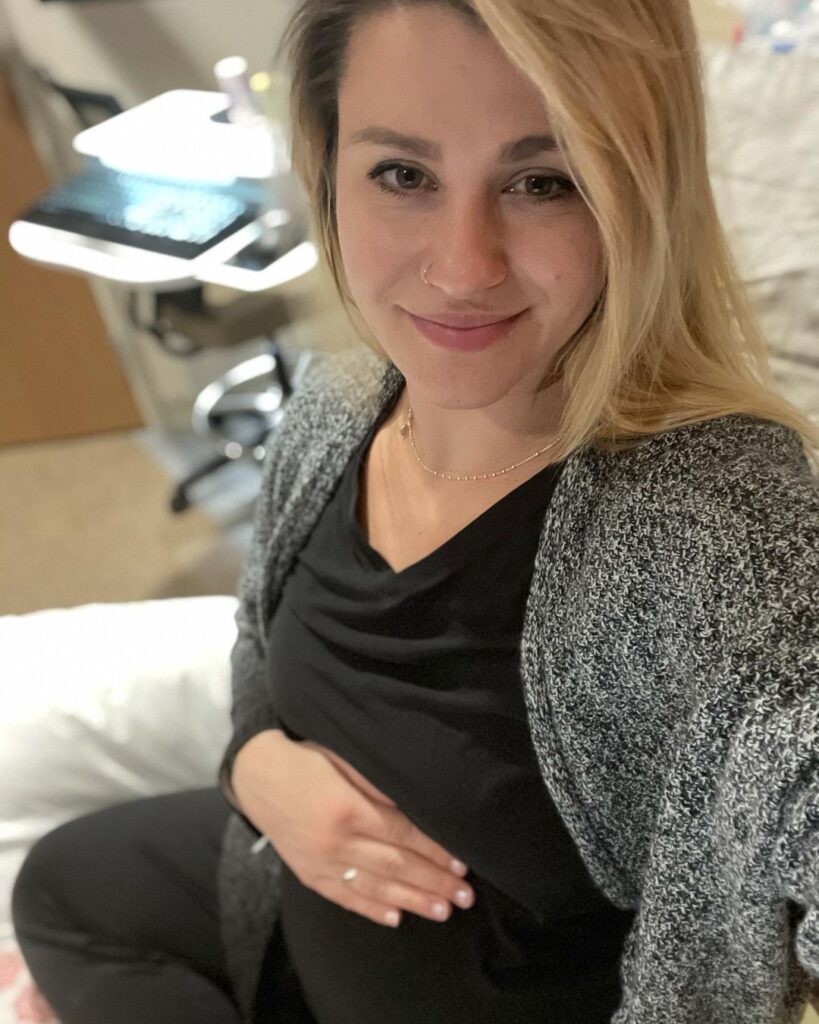
The first week was so excruciating, I almost walked out. I sobbed and pleaded each day to see my son and fought tooth and nail for visitation only to be granted two times a week outside for 20 minuets. That first week I was hooked up to NST’s 3x a day for 3 hours each day and routine ultrasounds twice a week. The twins were measuring close to one another in size and weight and I received steroid shots to help develop their lungs. The boys were looking good regardless of my emotional state. Despite how miserable I was, I knew I was here for the right reasons. I started to feel at peace with my situation and that we would make it through as a family.
March 10th was a normal morning and I was excited because my son was coming to visit. I hopped on the NST scan early so I would be ready to see my son. Baby B was experiencing decals (drop in heart rate) but I wasn’t panicked because I knew it was common to experience decals naturally in utero. They called ultrasound to come down and take a look. The scans looked good, but they said I would have to be monitored more just to be safe. I told my mom to keep Easton at home for today and to try again tomorrow just in case.
When I saw the doctor walk into my room I knew things were not good. He causally said “we need to prep for c-section” like things were going to be just fine. I called Jack right away and couldn’t even utter the words to him on the phone. I just began to sob “the boys aren’t doing well you need to come” was all I could get out. Hearing your significant other sob on the other end of the line, but also trying to keep it together for you is something I can’t even explain.
I was only 26.4 weeks pregnant, it was too soon. I was in shock. Jack made it just as I was being wheeled into the OR. Jack wasn’t allowed in the OR while they prepped me for my c-section. All I could hear around me were the nurses yelling “we lost the heart beat” and the doctor yelling “scalpel, we are taking them now” like something straight out of a movie. I screamed where is my husband and poor Jack walked in as they were opening me up.
I just stared into Jacks eyes crying saying “its too soon it’s too soon”. At 10:30am on March 10th we heard two of the tinniest cries imaginable as Hunter and Wade made their dramatic way into the world interlocked in each others arms. We were able to see them for a short moment before they were sent straight to the children’s hospital.

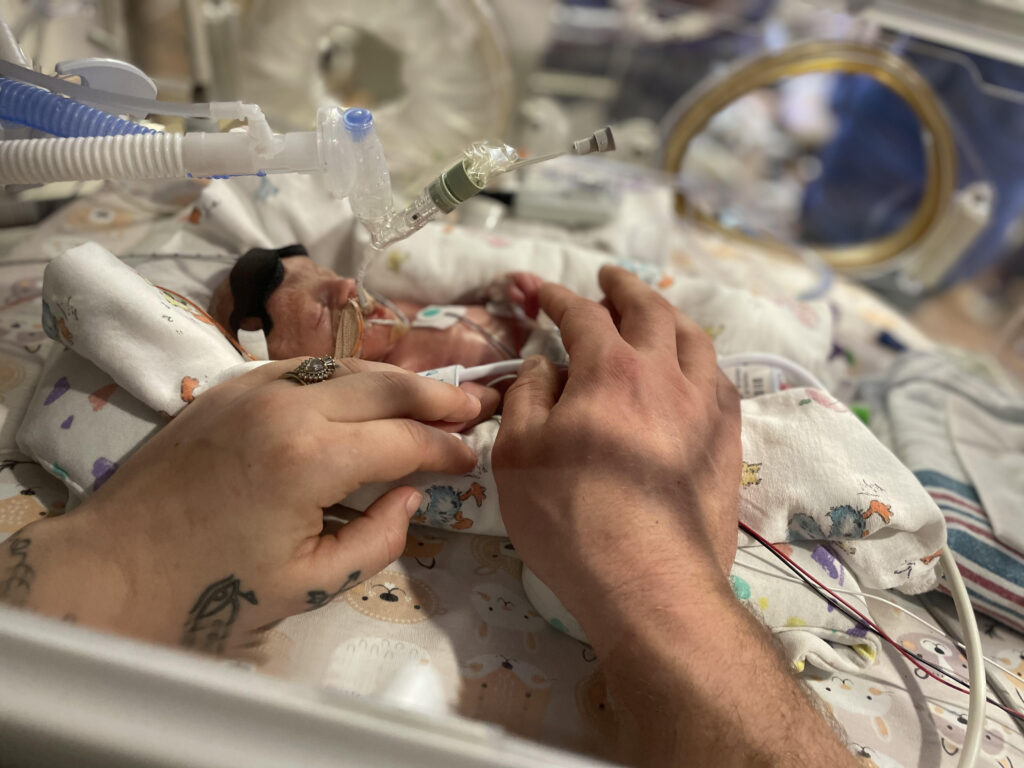
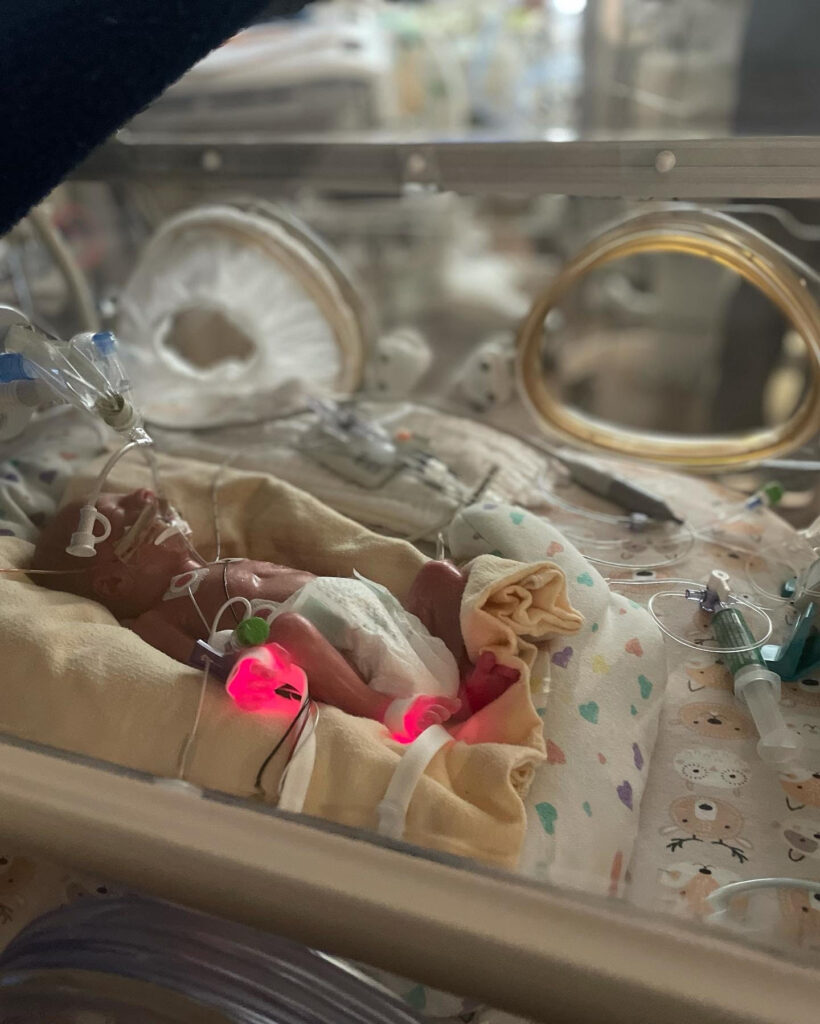
Recovering from an emergency c-section and not being able to be with my children is something I can’t put into words. Ten hours post surgery I left the hospital to go to the NICU, I stood for 12 hours post op just staring at my tiny helpless boys. My brain was in a fog and I was so worried they wouldn’t make it.
On top of the boys being born at 26 weeks twin B, our sweet boy Wade was diagnosed with Hemifacial Mircosomia (Hemifacial” means one side of the face. “Microsomia” means smallness). Even with all of my ultrasounds this was never detected.
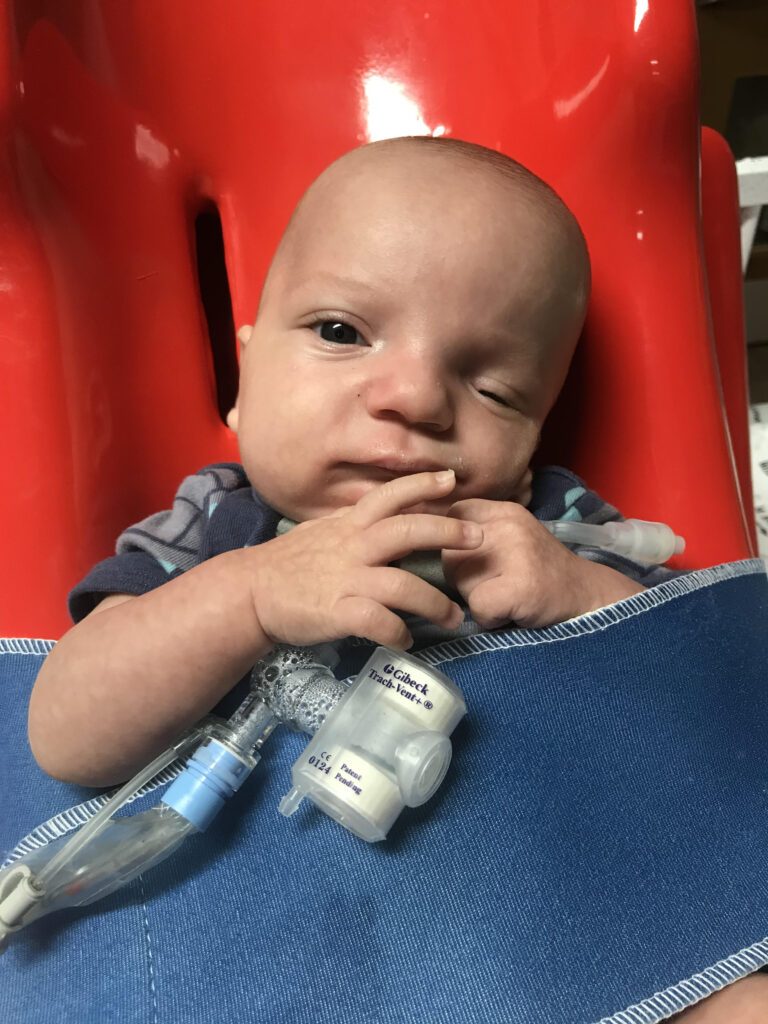
The next 5 months came with more complications imaginable. Both boys suffered from pneumonia twice, 5 Staff assists, 8 different types of antibiotics, numerous pulmonary hemorrhages, 5 failed extubations, 4 picc lines, 5 mid lines, 4 isolations (resulting in the boys being separated for months) and countless IV’s. Unfortunately after Wades 3rd failed extubation it was ruled that his lungs were okay, but due to his lack of jaw the soft tissues in his face was blocking his airway resulting in a tracheotomy and G-tube procedure.
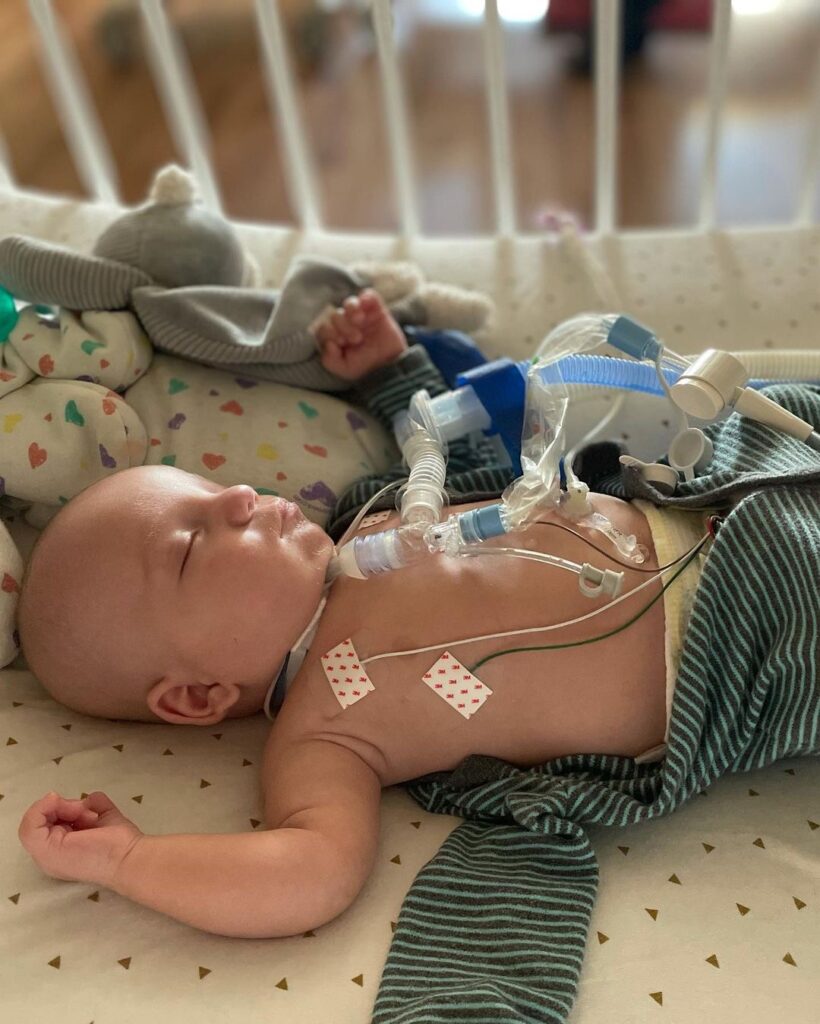
Hunter got sick early into his time in the NICU which really damaged his lungs. The first round of steroids failed and it wasn’t until 44 weeks that a second round of steroids helped Hunter. Wade has healed well post op and my husband and I are learning how to take care of him and making accommodation on when he can come home with us, but due to him having a tracheostomy’s we are required to have 24 hour care.
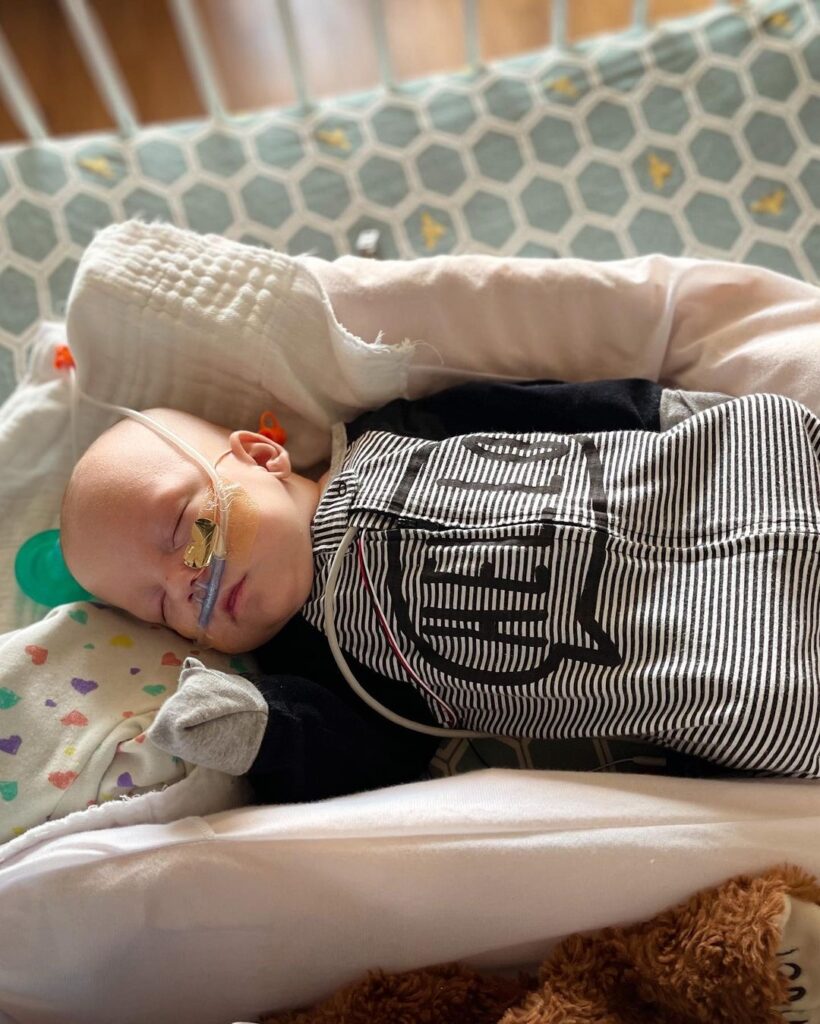
Easton (my 18 month old) has yet to meet his brothers, but prays for them daily. We even FaceTime with them so he can see the twins. For four long months it felt like we would never see better days. I have never prayed so hard in my life, why wasn’t God doing something? Where was he? I asked. God was their all along and continues to preform miracles on my boys, maybe not in the way I wanted but they are both here and strong each day! This last month has been nothing short of miraculous and we pray for continued progress for each passing day.
What was the hardest thing you went through during this time?
I think the hardest part was being in the darkest place in my life emotionally while trying to stay strong for my husband and children. It was also so hard trying to be at the NICU enough and also trying to be home enough for Easton. Mom guilt in every direction. There is nothing more painful than to see your children struggle and not be able to help them. I couldn’t take their pain away. There were times they we so unstable that I felt that holding them would cause more harm than good. I was able to provide milk for the first two months, but once the boys both where critically ill the stress plummeted my supply.

What advice do you have for people going through a hard time?
My advice for going through a hard time is one moment at a time, as corny as that sounds. Taking each medical diagnosis at a time, each bad phone call at a time. Lean into your faith and your significant other and ask for help. Remember that it is also okay to take time to yourself to process and mourn your situation. I am 5 months into our NICU journey and never thought we would be where we are!
What helped you the most during this hard time?
What helped us the most during our trial was God and our amazing community. The support and prayers for our family were beautifully overwhelming. We truly still couldn’t and still can’t do it without our loved ones who help us manage our home life and NICU life. One musical group that I listened to the most and helped me through a lot of emotional drives to and from the NICU is Maverick City Music and Bryan and Katie Torwalt.

Share an update on your life now
Currently our boys just celebrated 5 months in the NICU, this is the first time I have celebrated a month milestone because we just never had good news to share. Wade is stronger each day and weaning off his vent to the point where we have started HME trials 2x a day for 30 minuets, increasing the time as he tolerates it. The medical team thinks that he might not need a ventilator during the day and potentially only at night time if that! This is best case scenario. We have mapped out what Wades future procedures will look like to correct his Jaw, eye, and ear, but we will need to wait till he is older (3-5). Hoping the jaw surgery will correct his airway complication and can have his tracheostomy removed!
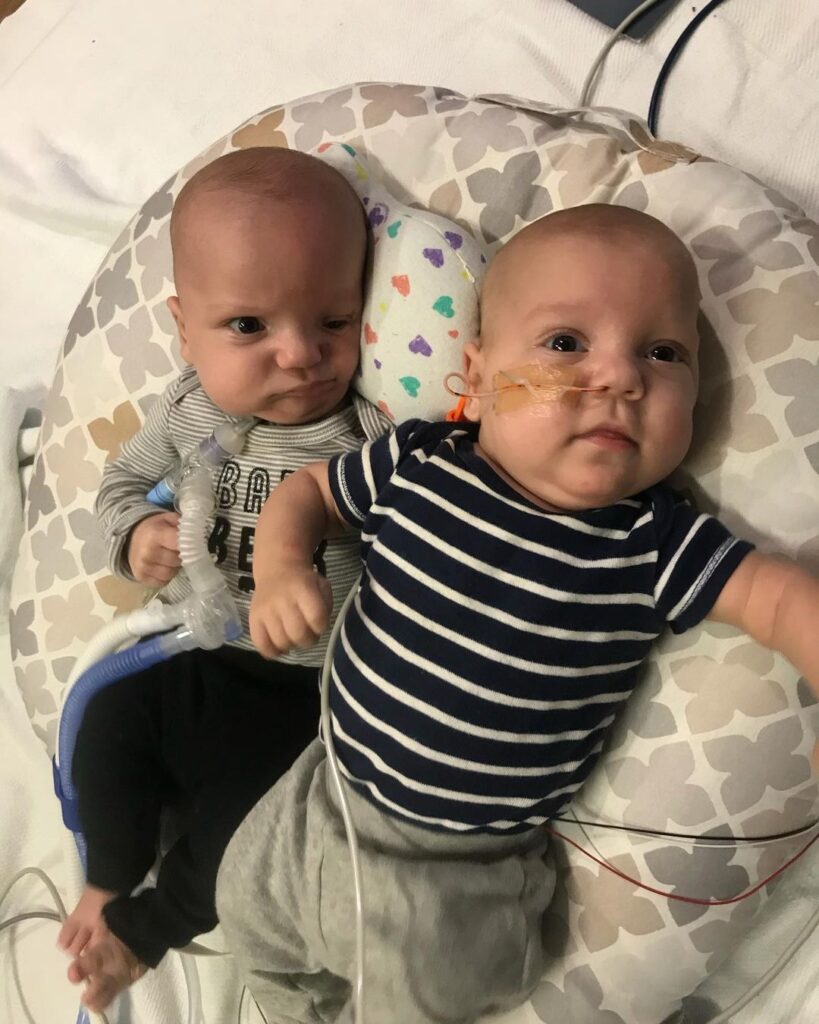
Hunter is currently on a 8-10 week coarse of steroids that have helped him with his extubation he is no longer on the vent and at 2.0 on Vaportherm and 21% oxygen most of the day. The team is going to try and see how he does without it to determine whether or not he will need low flow oxygen to come home on. Once he is stable with oxygen we can begin attempting bottle feeds. After 5 months we have yet heard the word “Discharge” yet for either of the boys, but I know that they are in the best care and when their time to come home happens we will be thrilled but until then we are continuing to make the best out of this situation for our family. The road ahead is uncertain but each day our family grows closer in many ways.


Shannon you are doing great. All three of the boys are beautiful. I hope within the next couple months you will hear the word discharge and your life will start all over again in a different kind of madness. Praying for all of you